Local News
A narrow 10–7 vote ended GLP-1 coverage for state employees, citing high premium costs and a tight state budget.
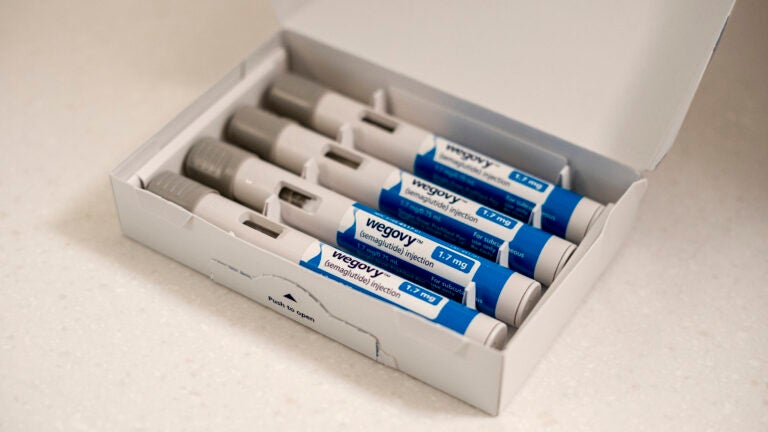
The commission that oversees health insurance for state employees has voted to end coverage of GLP-1 drugs for weight loss, a decision driven by soaring costs that officials say are straining the state budget.
In a 10-7 vote last Thursday, the Massachusetts Group Insurance Commission, which covers more than 460,000 people, agreed to drop the benefit, joining commercial insurers such as Blue Cross of Massachusetts, Point32Health, and Health New England.
Commissioners who opposed the move warned it could deepen health disparities and potentially raise costs later if members with chronic conditions worsen.
Roughly 22,000 GIC members currently take GLP-1 medications for weight loss, costing the state about $46 million, according to Margaret Anshutz, the agency’s director of health policy and analytics, at the meeting.
The pressure of rising drug spending prompted the governor to ask the commission to find about $100 million in savings.
While the GIC weighed broader cost-cutting measures, including higher co-pays and deductibles, Gov. Maura Healey urged commissioners last week to scrap most of those proposals and instead move ahead only with ending GLP-1 coverage for weight loss.
Dana Sullivan, the board’s designee from the Executive Office for Administration and Finance, said the move is part of a longer-term strategy to give insurers more leverage with drugmakers.
“As the largest purchaser of health insurance in Massachusetts, we’re a crucial part of the effort,” Sullivan said. “If we cut coverage collectively, we have market power to push those prices down to get access for our membership.”
Eliminating the benefit is expected to bring premium growth down to an average of 7.5%, the smallest increase in years, she said.
The vote comes as pharmaceutical giants such as Novo Nordisk and Eli Lilly lower prices on their injectables and a new oral version amid intensifying competition, though monthly costs still reach into the hundreds of dollars.
“These drugs are expensive, but they’re also life-changing,” said Anshutz, adding that weight often returns within 18 months once patients stop using GLP-1s. She warned that ending coverage will disproportionately affect lower-income members who can’t afford to pay out of pocket.
Commissioner Melissa Murphy-Rodrigues said she fears the coverage may never come back, even if prices fall. “For me, it’s like what’s next?” she said. “Is it EpiPens? Is it epidurals? What are we going to decide is not worthy of being insured?”
The Massachusetts Teachers Association also urged the state to continue coverage of GLP-1 medications.
“Health care in this country is broken, but asking public employees to pay more is not the solution,” President Max Page and Vice President Deb McCarthy said in a joint statement. “MTA members will continue to fight for affordable access to GLP-1 medications that have been life-changing for so many people.”
Sign up for the Today newsletter
Get everything you need to know to start your day, delivered right to your inbox every morning.

